The Duality of Workforce Stabilization
J.P. Morgan 2026


By Frank Stevens and Steve Wasson
After years of volatility, hospitals and health systems nationwide are seeing signs of workforce stabilization. That was a consistent theme at this year’s J.P. Morgan Healthcare Conference, Not-for-profit Track. Every year in January, healthcare leaders from across the industry converge on San Francisco to hear how the nation’s largest health systems are responding to emerging industry challenges and opportunities. The high-energy event provides a wealth of valuable insights, as top health system leaders share their organizations’ latest performance data and strategic priorities for the year ahead.
This article is the first in a three-part series in which Strata explores key takeaways from the conference, combined with findings from our proprietary hospital and health system performance data, and learnings from ongoing discussions with healthcare executives from a broad range of organizations.
At the J.P. Morgan conference, C-suite leaders touted trends of enhanced employee retention and engagement, a reduced reliance on contract labor, and more consistent staffing models. In addition to these operational wins, leaders emphasized that a more stable workforce underpins better care delivery and stronger financial performance.
Yet, while greater workforce stabilization is helping moderate many pressure points, it does not necessarily equal relief. While overall non-labor expense growth outpaced labor expenses throughout 2025, labor costs continue to rise and remain a dominant pressure for health systems nationwide, according to Strata data from more than 1,850 hospitals nationwide. The result is a dual reality: organizations are better staffed and less dependent on premium labor but, at the same time, the costs associated with maintaining that stability in an intensely competitive labor market continue to rise.
Stability gains and the cost trade-off
Health systems have made clear progress in shifting away from their reliance on contract labor, which spiked due to widespread shortages during COVID-19 pandemic. Use of contract labor and related expenses has declined significantly in recent years, as shown by Strata data. From 2023 to 2025, median contract hours per adjusted patient day decreased 29% for health systems nationwide, while contract labor expense per adjusted patient day dropped 31% over the same period.
At the same time, worked hours per adjusted patient day have remained relatively stable. This dynamic suggests that contract hours have largely shifted back to employed staff, without a measurable change in labor efficiency in either direction.

Get an in-depth look at current healthcare trends with analyses of financial, operational, and claims data from organizations nationwide, with insights drawn from all of Strata’s datasets.
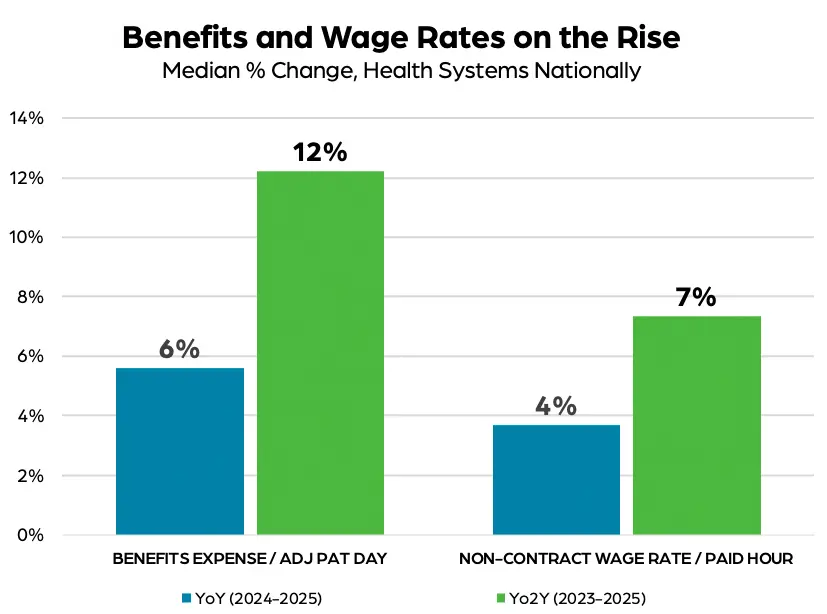
However, the financial benefit of this shift has been muted. Total labor expense continues to climb as organizations reinvest savings from reduced contract labor into higher wages, benefits, and retention incentives for employed staff. Median health system wages paid to non-contract workers increased 7% and benefits expense per adjusted patient day rose 12% from 2023 to 2025, according to Strata data.
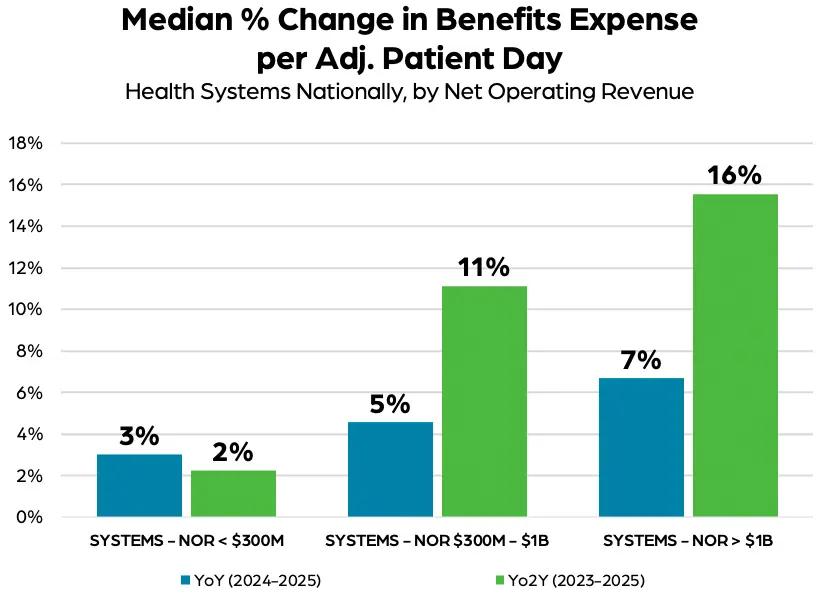
While such expenses rose for all health systems, the pace of increases varied by organization size. For example, benefits expense per adjusted patient day rose 2% over the two-year period for health systems with a net operating revenue (NOR) less than $300 million, but 11% for those with NOR of $300 million to $1 billion, and 16% for those with NOR greater than $1 billion.
In Strata’s discussions with healthcare leaders, executives cite these rising costs as a significant concern, with some reporting multiple consecutive years of wage hikes as high as 6% per year, contributing hundreds of millions of dollars in added expenses. One leader noted the structural imbalance succinctly, saying his organization faced “2% reimbursement increases versus 7% pay raises.”
This dynamic is reflected broadly across the industry. In Strata’s latest annual survey of hospital and health system finance leaders, roughly half of respondents identified labor as one of their top two concerns heading into 2026.
Workforce stability as a care and performance strategy
Despite ongoing expense pressures, the strategic case for workforce stabilization is stronger than ever. Throughout the J.P. Morgan conference, leaders consistently tied staffing stability to quality,
safety, and enhanced operational performance. The conviction was clear: stable teams deliver better care.
Leaders from numerous health systems shared recent strides in workforce stability. A Midwest-based health system described talent as its “primary differentiator,” a philosophy the health system supports through sustained investment in compensation, development, and enhancing the workplace environment. The organization reported that employee net promoter scores have doubled over three years, while average tenure is now three to four times that of industry norms.
Others emphasized the role of technology in reinforcing workforce stability. One health system reported more than a million hours saved in 2025 through digital and artificial intelligence (AI)-enabled efficiencies, alongside declines in contract labor, overtime, and full-time equivalents (FTEs) per adjusted occupied bed as case mix complexity increased. Leaders from another health system highlighted the organization’s electronic health record (EHR) system migration, ambient documentation, and AI-driven workflow tools as part of a broader commitment to automate administrative burden wherever possible by 2028.
Right-sizing, productivity, and governance
In Strata’s annual survey, finance leaders ranked reducing costs and improving productivity measurement among their top priorities for 2026. Respondents pointed to better productivity reporting, more effective use of labor benchmarks, and real-time, shift-level productivity analysis as the most impactful strategies for managing labor expenses.
In Strata’s regular meetings with hospital and health system leaders, executives say they are focused on “right-sizing” the workforce. Organizations are recalibrating staffing models post-COVID, with greater emphasis on position control and productivity governance. While contract labor costs have come down, productivity variation, premium pay, and recruitment challenges remain structural issues.
Leaders acknowledge cultural barriers. Productivity data is widely viewed as essential but often under-trusted, with resistance rooted in concerns about fairness, context, and clinical autonomy. Overcoming that resistance will require not just better analytics, but clearer governance, transparency, and alignment between operational leaders and frontline teams.
Long-term strategies in a constrained market
Labor remains the dominant cost driver for hospitals, accounting for approximately 56% of total hospital expenses.i As such, it will always be at the forefront of health system improvement strategies. Looking ahead, executives stressed a need to invest in long-term workforce supply strategies, including education and training pipelines. For example, WellSpan Health partnered with Jersey College to establish a nursing school in southern Pennsylvania with the goal of helping to address workforce shortages.ii
Recent moves toward stabilization have delivered meaningful benefits in care quality, engagement, and operational consistency for many health systems. At the same time, rising wages and benefits have locked labor costs into a structurally higher baseline, demanding more disciplined productivity management and governance. Healthcare leaders also are increasingly shifting their focus on labor beyond clinical settings, emphasizing a need to reduce corporate services spend, optimize spans of control, and relentlessly prioritize how they are investing in talent.
For healthcare leaders, the challenge in 2026 and beyond will be navigating this duality: sustaining a stable, engaged workforce while rigorously managing labor productivity and expenses. Those that succeed will not treat labor solely as an expense to be contained, but as a strategic asset that requires data-driven oversight, cultural alignment, and long-term investment.
The American Hospital Association: The Cost of Caring: Challenges Facing America’s Hospitals in 2025. April 2025.
ii WellSpan: “WellSpan Health Partners with Jersey College to Establish a School of Nursing.” The WellSpan Spotlight, June 11, 2024.


