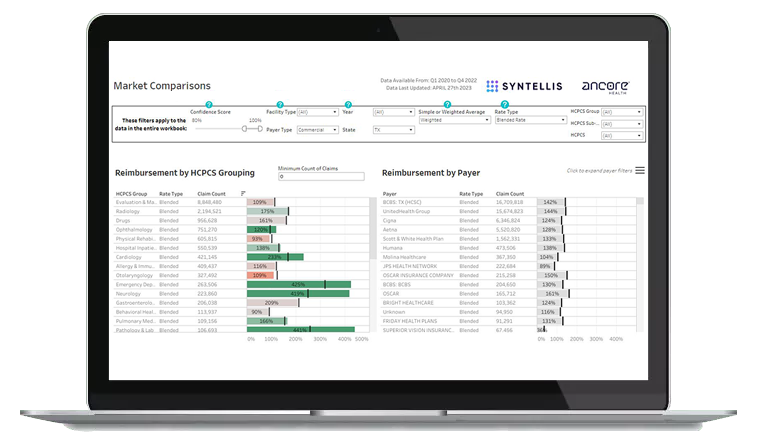
Market Reimbursement Analyzer
Maximize reimbursement rates with market-specific intelligence
Negotiate reimbursements confidently
With unprecedented transparency into reimbursement rates, Axiom Market Reimbursement Analyzer makes it easy to objectively compare rates and equips healthcare leaders to negotiate fair reimbursement with payers.
Analyze ROI potential and improve forecasting
Champion growth and acquisition targets with the highest potential of success. Market Reimbursement Analyzer leverages proprietary 835 All-Payer Claims Data (APCD) to analyze market rates by payer, provider, CPT code, and/or service line to deliver insights into your financial opportunity. This makes it easy to assess the revenue potential of entering new markets, forecast future revenue, and view market reimbursement rate trends over time to accurately gauge revenue growth potential.
Objective Market & Provider Comparisons
Curated and easily accessible state, market, and product line data help you better understand providers’ reimbursement trends and your risks and opportunities. Evaluate reimbursement rates at a granular level, including office visits, surgical procedures, and diagnostic and therapeutic services, as well as services at outpatient hospitals and ambulatory surgical centers.