Operational Rigor as the Foundation for Recovery and Growth
J.P. Morgan 2026


By Frank Stevens and Steve Wasson
Over the past several years, health system leaders have spoken candidly about disruption, uncertainty, and recovery. At this year’s J.P. Morgan Healthcare Conference, Not-for-profit Track, the tone was notably different. Executives were explicit about moving beyond episodic cost-cutting initiatives to something deeper and more durable: operating rigor as the foundation for sustained performance, margin recovery, and long-term growth.
As executives from the largest health systems presented their priorities for the year ahead, a common thread emerged. Organizations that are stabilizing and moving forward are not relying on one-time cost programs or isolated technology pilots. They are building disciplined and sustainable operating models, clear accountability, and repeatable execution supported by data, robust decision support systems, and increasingly, artificial intelligence (AI) embedded directly into workflows.
This article concludes a three-part series in which Strata examines key themes from the conference alongside insights from our proprietary hospital and health system performance data and ongoing conversations with healthcare leaders across a range of organizations.
Throughout the conference, healthcare leaders emphasized that recovery and financial stability only endure when operating rigor becomes the baseline. A health system based in the Midwest articulated a “flywheel” model of volume and mix improvement, capacity and cost discipline, and stronger commercial competitiveness reinforcing one another over time. Operating discipline was presented as the foundation and the permanent engine underlying all strategy across its multi-state service area.
Leaders from another health system echoed a similar message, describing a disciplined financial turnaround and strategic reset that repositioned the organization from a loosely connected healthcare conglomerate into a focused, diversified healthcare system across seven states. Leaders highlighted a regimented operating cadence, including weekly one-hour operating reviews with the system’s top 75 leaders and dozens of tightly tracked workstreams spanning revenue, expense, access, and portfolio actions. The results were tangible, including a significant reduction in use of agency labor and sizable savings in shared services.
An analysis of Strata data shows some improvements in core operational metrics for hospitals nationwide. For example, median length of stay has remained stable at approximately three days over the past three years, indicating overall consistency in inpatient throughput and care delivery. Case mix index (CMI) has also been relatively stable in recent years, with median year-over-year changes hovering near 0% from 2023 to 2025, suggesting a stable acuity profile. In 2025, the median change in CMI was down 0.59%, reflecting strategic shifts toward lower-acuity outpatient care.
At the J.P. Morgan conference, leaders consistently highlighted the importance of operating models, cadence, and accountability down to the supervisor level. Sutter Health described its transformation from a fragmented holding company into an integrated operating organization through a “ONE Sutter” model, built around a unified digital platform, consistent operating rhythm, and integrated capital planning.i Operating rigor is pushed deep into the organization, with “everyone knowing their numbers,” reinforcing an ingrained and continuous cycle of access, growth, margin, and reinvestment.
Another health system similarly framed optimization as a core management discipline. Standardizing and simplifying operational processes were positioned as durable sources of savings and scalable performance improvement, enabled by technology modernization and a unified operating backbone.
One of the most striking shifts at this year’s conference was how leaders talked about AI. Just a few years ago, AI was framed largely as pilots and proofs of concept. In 2026, it is increasingly described as embedded infrastructure producing measurable outcomes.
Strata’s data reflect this shift. The percentage of health systems listing roles that include AI in the job description more than doubled, while the average number of AI full-time equivalents per system more than tripled over the same period. These roles span management and frontline functions, from analysts and project managers to vice presidents and chief officers, signaling institutional commitment rather than experimentation.
Health systems provided concrete examples. Intermountain Health highlighted AI tools embedded into its electronic health record environment, including AI-enabled triage of tickets.ii Leaders from Cleveland Clinic described AI as infrastructure across three domains: patients, caregivers, and enterprise operations, supported by deep technology integration and partnerships. The health system’s partnership with Palantir Technologies, for example, enables caregivers to leverage AI to better view, manage, and forecast bed availability, patient demand, staffing, and operating room scheduling.iii
Inova Health System presented AI as operational connective tissue. Leaders highlighted an AI-enabled call center handling over 300,000 calls per month, with half of appointment changes managed autonomously, unlocking more than 4,000 labor hours monthly and delivering an eight-times return on investment.iv
Executives from another health system positioned AI as a core engine for clinical excellence, research acceleration, and education. The organization is using AI in a wide range of applications, including to support precision oncology and early cancer detection, and helping to build care planning models to drive clinical workforce efficiencies.
Another consistent theme was the reframing of performance improvement itself. Leaders repeatedly rejected the idea of episodic cost cutting in favor of performance improvement as a permanent organizational capability.
One health system, for example, emphasized its repeatable global operating model and codified management system. Another health system’s focus on execution cadence, KPI transparency, and portfolio discipline reinforce the same principle: improvement is continuous, governed, and embedded in leadership routines.

Get an in-depth look at current healthcare trends with analyses of financial, operational, and claims data from organizations nationwide, with insights drawn from all of Strata’s datasets.
 This shift places renewed focus on effective performance management and decision support systems. As operating complexity increases and AI becomes more deeply integrated, healthcare leaders need real-time visibility into operational performance and clear accountability for action. Technology advancements were consistently framed as foundational enablers of simplification, standardization, and scalable execution.
This shift places renewed focus on effective performance management and decision support systems. As operating complexity increases and AI becomes more deeply integrated, healthcare leaders need real-time visibility into operational performance and clear accountability for action. Technology advancements were consistently framed as foundational enablers of simplification, standardization, and scalable execution.
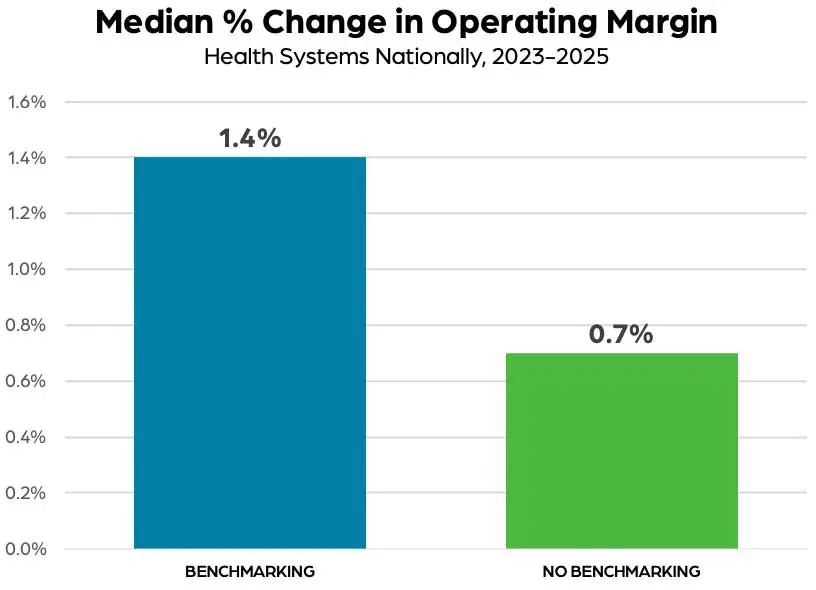
 While definitively identifying cause and effect in complex systems is difficult, a high-level comparison of organizations that use benchmarking tools versus those that do not seem to support the importance of having rigorous operating processes. An analysis shows that health systems that used a benchmarking solution to routinely monitor and compare key performance metrics saw greater improvements over time in operating margins, total expenses,
While definitively identifying cause and effect in complex systems is difficult, a high-level comparison of organizations that use benchmarking tools versus those that do not seem to support the importance of having rigorous operating processes. An analysis shows that health systems that used a benchmarking solution to routinely monitor and compare key performance metrics saw greater improvements over time in operating margins, total expenses,
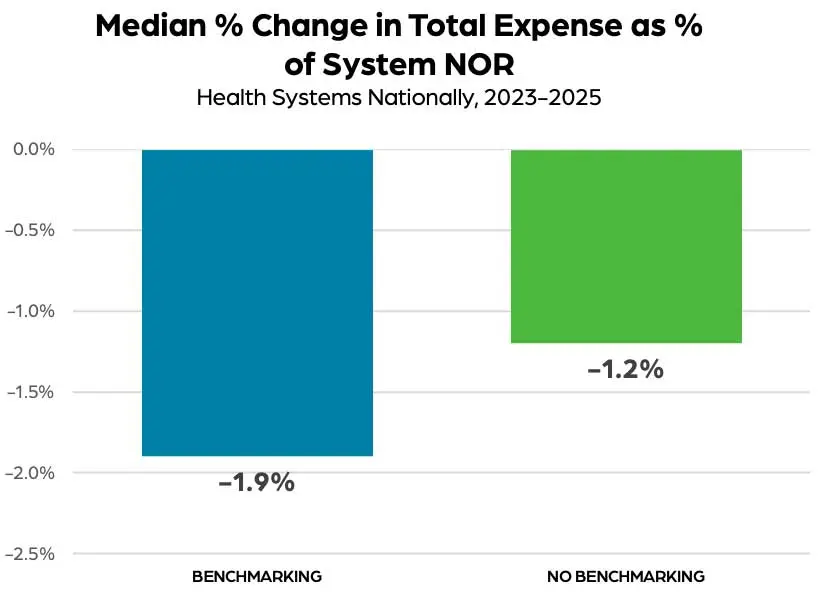
and productivity in recent years versus their peers. From 2023 to 2025, for example, health systems that used a benchmarking solution saw median change in operating margin increase 1.4 percentage points compared to an increase of just 0.7 percentage point for health systems that did not. Similarly, health systems that used benchmarking saw median change in total expense as a percent of system net operating revenue decrease 1.9% over the two-year period versus a 1.2% decrease for non-users.
Perhaps the most significant change came in the form of productivity. Health systems that use benchmarking saw median percent change in worked hours per adjusted patient day decrease 1.0% from 2024 to 2025 versus a 1.8% increase for non-users over the same period.
Results will always vary by entity, but these analyses suggest that healthcare leaders that use benchmarking tools appear to be more effective at driving meaningful operational improvements for their organizations.
Taken together, the message from the J.P. Morgan Conference was clear. Operational rigor is essential for growth. Systems that are improving access, optimizing capacity, and embedding disciplined execution are creating the financial and organizational flexibility to reinvest, pursue strategic acquisitions, and expand into new care models.
Healthcare leaders repeatedly emphasized the need to build durable operating engines where data, accountability, and AI reinforce one another. In a sector still facing structural pressure, operational rigor has become the most reliable source of resilience and the clearest path to sustainable growth.
i Sutter Health: 2024 Annual Report: Momentum with Purpose. August 2025.
ii Bresnick, J.: “Responsible AI Governance Is Helping Intermountain Face the Headwinds.” DHI Insights, Oct. 17, 2025.
iii Cleveland Clinic: “How AI Assists with Staffing, Scheduling, and Once-Tedious Tasks.” Feb. 14, 2024. \
iv Hyro: “Inova Health Hits 8.8x ROI with 100% Coverage of Patient Access Calls in First 6 Months.” 2025.


