Long-Term Health of Patients, Hospitals at Stake as Care Delays Continue
March 29, 2022
As federal relief funds dwindle and volumes remain stagnant, concerns mount about how providers will fare, especially those lacking robust outpatient services.
This is part of a series on hospital operations two years into the COVID-19 pandemic. Follow them here.
The slowdown of the COVID-19 pandemic in the U.S. has done little to speed up Americans’ return to healthcare.
Two years into the pandemic, healthcare experts are “very concerned” that patient volumes have yet to return to normal. That’s because people continue to delay important screenings and care, raising concerns about the long-term implications for patient health and the effect on the nation’s health system.
The downturn in patient care has been widespread with volumes still trailing in settings and services ranging from inpatient to outpatient care, emergency room visits and even cardiac care, according to data from healthcare vendor Strata. It analyzed data from more than 170 health systems, representing more than 1,100 hospitals across the country including academic medical centers and children’s and rural hospitals.
For the past two years, even amid the outbreak of COVID-19, patient foot traffic still fell below pre-pandemic levels, underscoring just how many people stayed away from hospitals and other traditional healthcare settings.
Some expected a sizable rebound in deferred care after visits plunged in 2020, but it never materialized to that extent. It’s left some to wonder when the pendulum will swing back in the other direction.
“The scary part that we haven’t started talking about yet is what that means five years from now,” said Sarah Alwardt, practice director for the Center for Healthcare Transformation within Avalere, a Washington D.C.-based consulting firm.
Patient volumes are still ‘in transition’
Even though COVID-19 sent hundreds of thousands in the U.S. to hospitals and stretched hospitals thin, inpatient volumes still fell markedly.
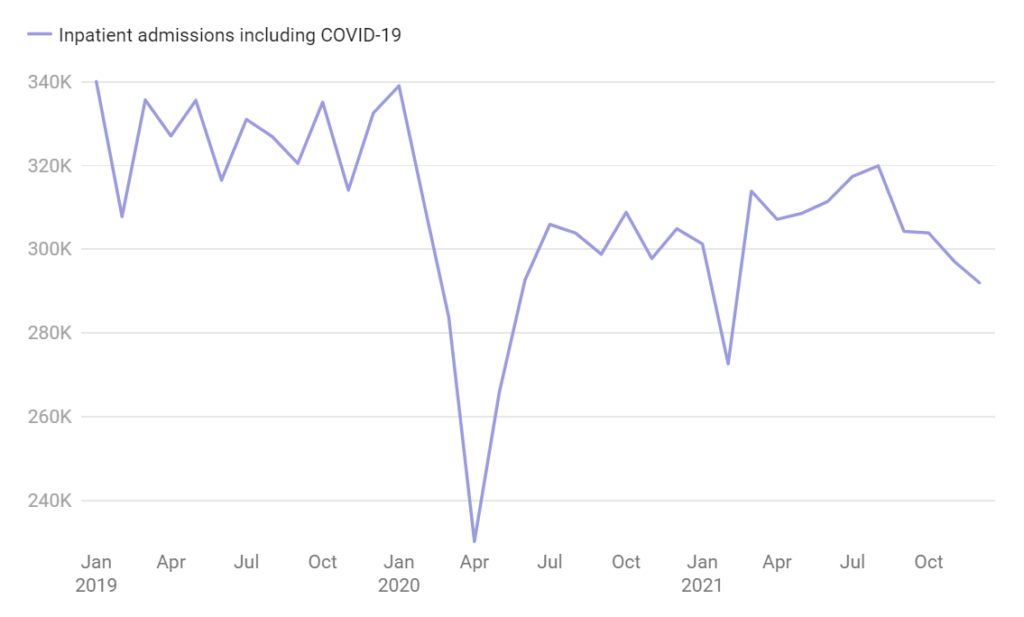
Inpatient admissions, including for COVID-19, dropped 9.7% in 2020 and 7% last year. Excluding patients with the virus, admissions slid 14.9% and 14% in 2020 and 2021, respectively, according to data from Strata.
Even amid the pandemic, fewer patients have been admitted to the hospital
Healthcare vendor Strata analyzed data from more than 1,100 hospitals across the country.
It’s not just hospital admissions. Fewer patients have turned up at emergency rooms, with declines of 21% and 15.5% in 2020 and 2021, respectively, according to Strata.
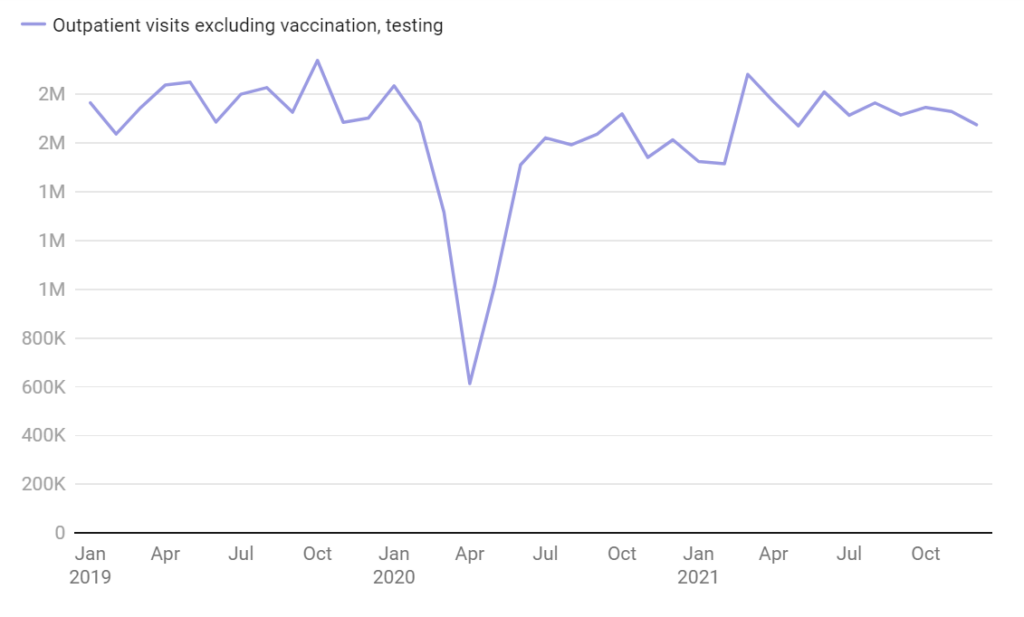
Outpatient visits, not including testing and vaccinations, also trailed historical levels. They fell 16.5% in 2020 and 3.2% in 2021.
Outpatient visits also declined during the past two years
Strata also analyzed the outpatient traffic of the more than 1,100 hospital systems it tracks, and even these more convenient visits for patients trail pre-pandemic levels.
“We’re seeing delays in care, or deferral of care, that we’re very, very concerned about,” Steve Lefar, executive director of data science at Strata, said in an interview.
Ever since the federal government declared a public health emergency in the spring of 2020, the virus, or the threat of it, has influenced patient behavior and created a drag on key patient volume metrics.
How volumes have fared throughout the duration of the pandemic is a topic Chris Mast and his colleagues at Epic Research have kept a close eye on. They have analyzed millions of healthcare claims to paint a clear picture of what has happened to healthcare utilization over the past two years.
They found many Americans have missed key screenings for cervical, breast and colon cancers. Although there has been much talk about the need to return to “baseline” — or normal volume trends evident in 2019 — what Epic Research’s analysis shows is that the nation has neither returned to baseline, nor has it made up for the screenings that were missed.
In order to catch up, the drop in missed screenings that fall below the historical trend would need to be mirrored above that baseline.
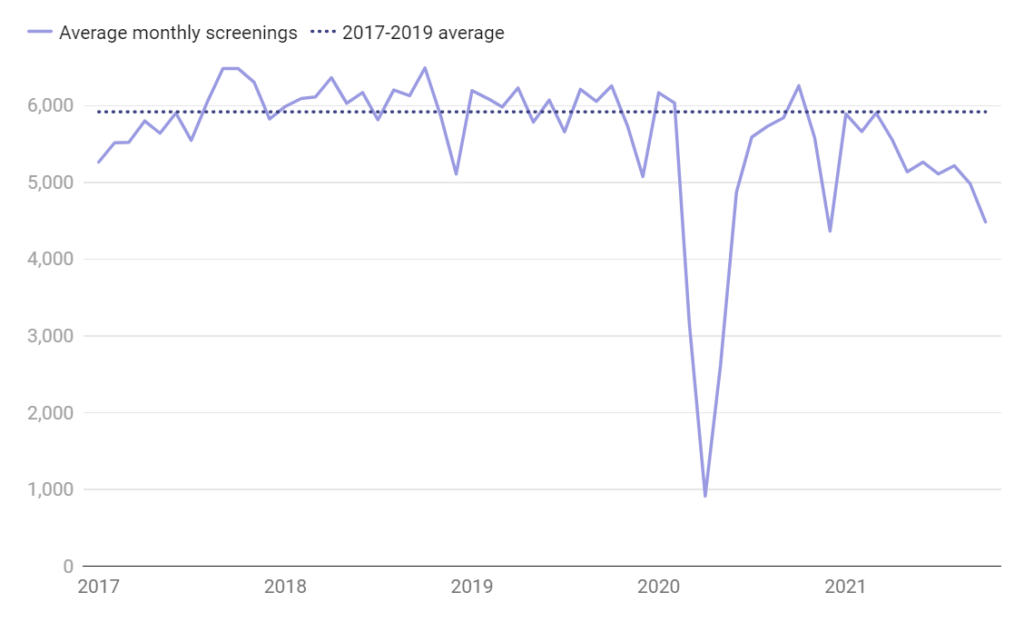
Patients continue to delay key screenings including cervical cancer
Screenings for cervical cancer were down 10% in 2021 when comparing the average weekly screenings to the historical average.
Mast and his colleagues are unsure a catch-up in screenings will happen, especially as more time passes. Still, patients are sensitive to messaging and every year there is a predictable bump in screenings during breast cancer awareness month, he said.
“What that tells me is that those messages have an impact,” Mast noted. With this in mind, organizations should be prodding patients to return for these annual checkups, he added.
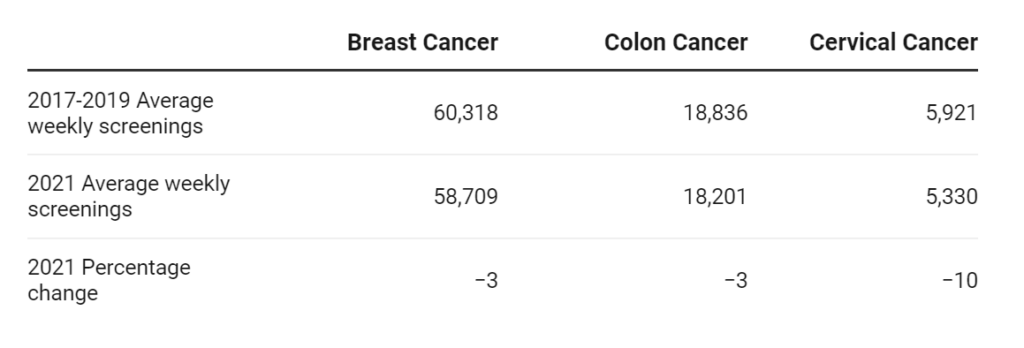
Across the board, cancer screenings have fallen, worrying experts
With targeted messaging, experts are hoping to see a rebound in screenings.
It’s not just cancer screenings. Emergency department visits have continued to lag throughout the pandemic. It’s a trend that has puzzled healthcare experts. What happened to all those health emergencies? Was it possible people were having fewer heart attacks and strokes?
Emergency room visits still lag pre-pandemic volumes
A constant laggard in key patient volumes has been emergency room visits, prompting researchers to examine why.
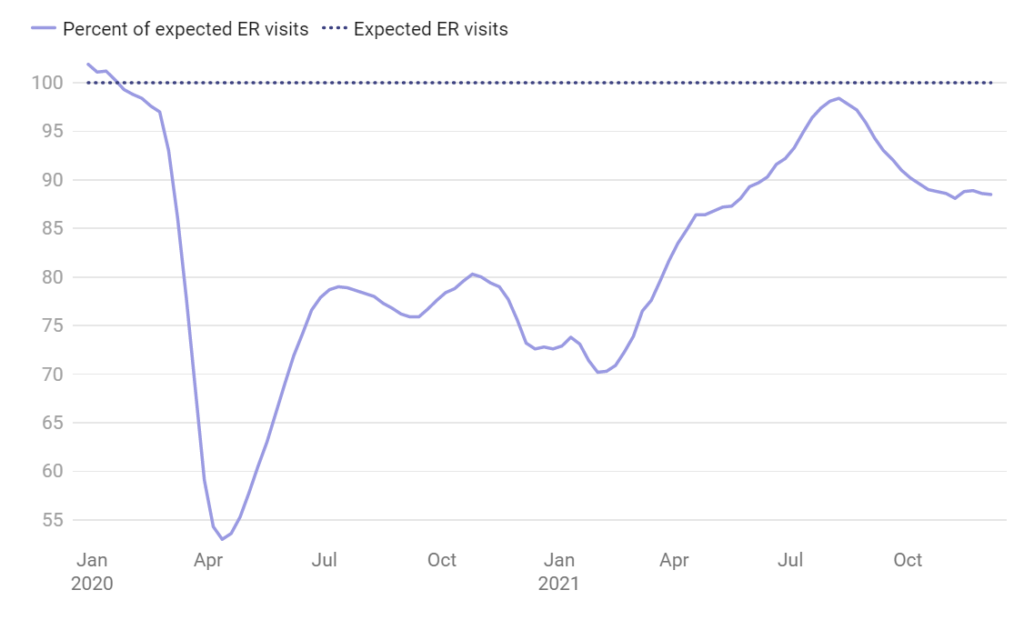
“It was perplexing. As we drilled into it, we saw that in some cases they didn’t really go anywhere,” Mast said.
The data show that higher-acuity patients, like those experiencing heart attacks and strokes, were coming to the ER at levels above the baseline, while lower-acuity patients were coming in at rates lower than 2019 levels.
“I would characterize the patterns of healthcare delivery, and people seeking healthcare, as being in transition. And we’re still waiting to see where those things are going to settle out,” Mast said.
Threat to hospitals
The decline in patient demand was so acute that the federal government funneled billions of taxpayer dollars to hospitals around the country to prop them up financially as operations were seemingly turned upside overnight.
As people deferred visits to the doctor and fewer were admitted to hospitals, it also meant insurers paid less for care than they were used to historically leading to record profits.
But as federal relief funds dwindle and volumes sag, it also raises concerns about how providers will fare financially.
The deflated volumes are occurring as hospitals grapple with increased expenses, particularly those tied to salaries and benefits as many have struggled to find enough staffing resources. During numerous COVID-19 surges, facilities have had to pay surging rates for traveling nurses in order to backfill shortages.
These operating challenges will continue to squeeze margins for many hospital operators, healthcare analysts have said.
At the same time, the pandemic has accelerated the shift of care to outpatient settings.
Inpatient orthopedic procedures have decreased dramatically over the past two years compared with 2019, according to Strata’s data. There has been a “massive shift” to outpatient facilities for these types of procedures, Lefar said, a service line that can be lucrative for many facilities.
The continued migration of services from inpatient to outpatient will pose challenges for some operators, especially those without robust outpatient offerings.
“The inpatient dependency is going to be a problem, there’s just no two ways about it,” Lefar said.
As healthcare executives consider how to move forward, experts such as Alwardt of Avalere say they need to think differently about how to interact with patients, especially after the meteoric rise in telehealth services.
“They’re so used to people coming to them,” Alwardt said.
Now, healthcare executives need to pivot their thinking to how can they proactively maintain those patient relationships, he added.
“This is going to take investment in a digital transformation that I don’t know if they counted on having to do,” he said.